In addition, previous papers have not revealed relationships between ΔPI-NRS and changes in the other above-mentioned clinical scales in the management of CLBP. However, clinical assessment of the utility of ΔPI-NRS specifically targeting CLBP patients has not been undertaken yet. 
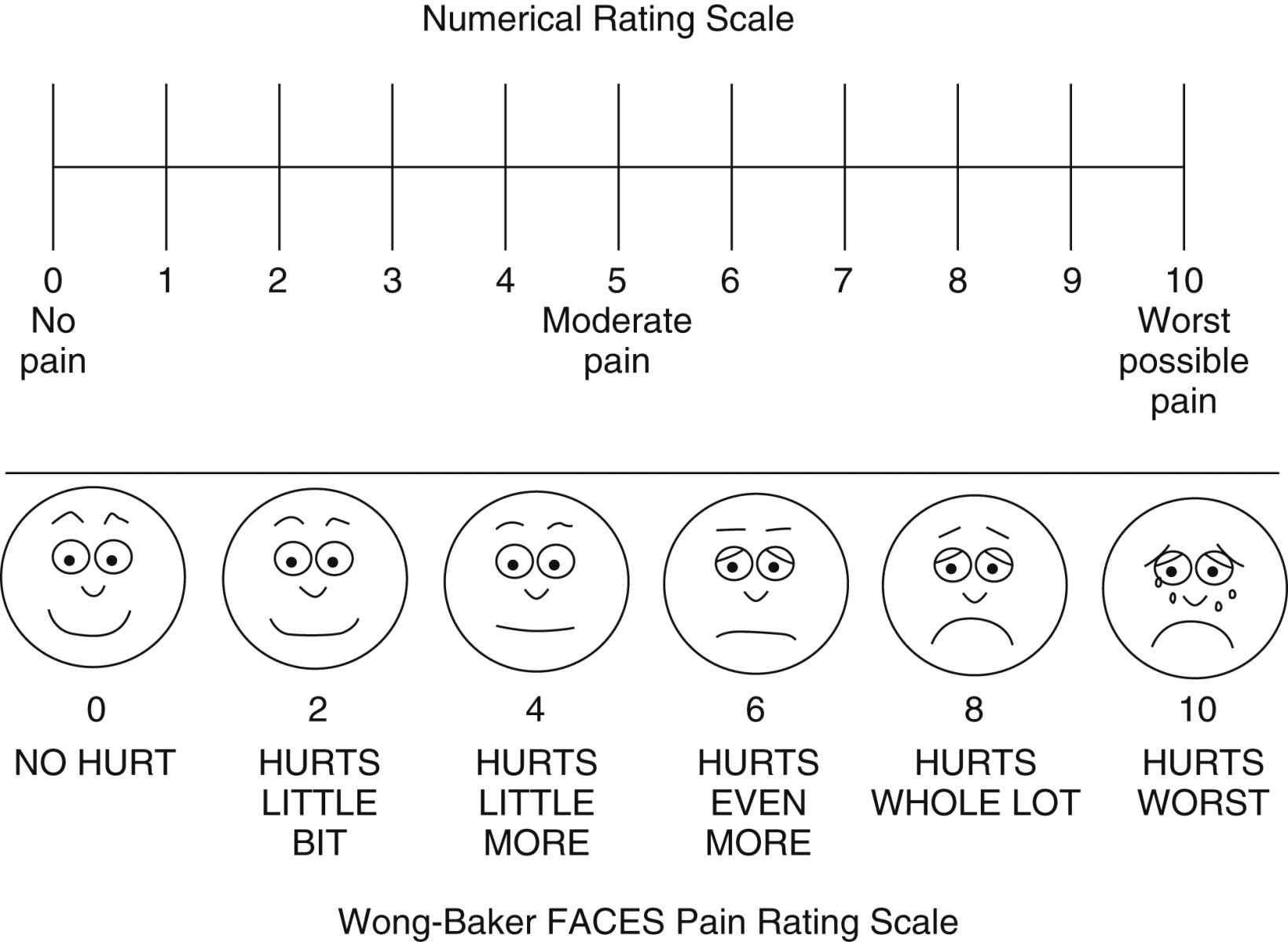
Besides, the utility of the cutoff value should be evaluated based on whether it exceeds a minimally clinically important difference (MCID), which can be defined based on the inherent variability of ΔPI-NRS. It has to be based on the patient’s global impression of change (PGIC) in pain intensity. However, an appropriate threshold (cutoff) value for ΔPI-NRS is not available for clinical use in the field of CLBP management. Therefore, although the PI-NRS itself is not so reliable for the objective assessment of pain intensity, post-treatment change in the PI-NRS (ΔPI-NRS) is generally considered useful in judging the effectiveness of a therapeutic regimen. Among these clinical scales, the PI-NRS is considered to be the most subjective one in that it depends on the sensitivity to pain of each patient. As additional tools in evaluating the status of chronic pain, many studies rely on patients’ self-administered answers to the questionnaires of various clinical scales, such as health-related quality of life (QOL) questionnaires, the Pain Disability Assessment Scale (PDAS), Hospital Anxiety and Depression Scale (HADS), Pain Catastrophizing Scale (PCS), and the Athens Insomnia Scale (AIS), a sleep disorder scale. In the management of CLBP patients, pain intensity is most frequently measured on the 11-point Pain Intensity Numerical Rating Scale (PI-NRS), which ranges from no pain = 0 to the worst possible pain = 10. In fact, even if a group of individuals receives the same stimuli or undergoes the same intervention, the rating of pain reported by the patients differs greatly. However, pain is a unique experience that no other person can feel or perceive on one’s behalf. It causes sleep interruption, fatigue, depressed mood, activity limitations, and restrictions in participation. These can be used as definitive indicator of therapeutic outcome in the management of chronic LBP patients.Ĭhronic low back pain (CLBP) has a major impact on the patient’s quality of life. Therefore, we determined cutoff values of these scales in distinguishing the status of ΔPI-NRS≥2 vs. Spearman’s correlation coefficient revealed close relationships between ΔPI-NRS and the six other clinical scales. The ΔPI-NRS cutoff value for distinguishing the PGIC status was determined by ROC analysis to be 1.3–1.8 depending on pre-treatment PI-NRS, which was rounded up to ΔPI-NRS = 2 for general use. We found ΔPI-NRS to be most closely associated with PGIC status regardless of pre-treatment pain intensity, followed by ΔEQ5D, ΔPDAS, ΔPSEC, and ΔPCS. 
Multivariate logistic regression analysis was performed to explore relevant scales in distinguishing the two groups. Patients were partitioned into two groups based on patient’s global impression of change (PGIC) three months after treatment: satisfied (PGIC = 1, 2) and unsatisfied (3–7). We included 161 LBP patients treated in two representative pain management centers. Its utility was compared with changes in six commonly used clinical scales in LBP patients: Pain Disability Assessment Scale (PDAS), Pain Self-Efficacy Questionnaire (PSEC), Pain Catastrophizing Scale (PCS), Athens Insomnia Scale (AIS), EuroQoL 5 Dimension (EQ5D), and Locomo 25. This study aimed to determine an objective cutoff value for a change in the Pain Intensity Numerical Rating Scale (ΔPI-NRS) three months after LBP treatment. Numerous clinical scales are available for evaluating pain, but their objective criteria in the management of LBP patients remain unclear. Low back pain (LBP) is the most common cause of chronic pain.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
